
Post-traumatic stress disorder (PTSD) and sleep have a complex, interconnected relationship that goes far beyond occasional bad dreams. Sleep problems in PTSD are actually considered part of the disorder, with hyperarousal and intrusion symptoms that can manifest as insomnia and nightmares. Understanding this connection is crucial for developing effective strategies to reclaim peaceful sleep.
PTSD nightmares are vivid, often traumatic dreams directly related to the original trauma that triggered the disorder. These experiences can cause intense fear, anxiety, and physical distress, sometimes waking the person in a state of panic. Unlike ordinary nightmares, PTSD-related dreams often involve exact replays of traumatic events and can feel devastatingly real.
Night terrors, while less common in adults, are episodes of intense screaming, fear, or physical movement while still asleep, followed by difficulty returning to rest. Among people who experience a traumatic event, those who suffer significant sleep problems appear to be more likely to develop PTSD in the future.
The Neurobiological Impact of Trauma on Sleep
Recent research has revealed that the pathophysiology exposes central dysfunction of brain structures at the level of the hippocampus, amygdala, and locus coeruleus, modulated by neurochemical imbalance in nor-adrenergic, dopaminergic, and serotonin pathways. This means that trauma literally changes how your brain processes sleep and dreams.
Key Brain Changes in PTSD:
- Hyperactive amygdala: Your brain’s alarm system remains on high alert, even during sleep
- Disrupted hippocampus function: Memory processing becomes fragmented, leading to intrusive dream content
- Altered neurotransmitter balance: Chemical messengers that regulate sleep cycles become imbalanced
- Elevated stress hormones: Cortisol and other stress chemicals remain elevated, affecting sleep architecture
Understanding that these changes are neurobiological responses to trauma - not personal weaknesses - can help reduce self-blame and encourage appropriate treatment seeking.
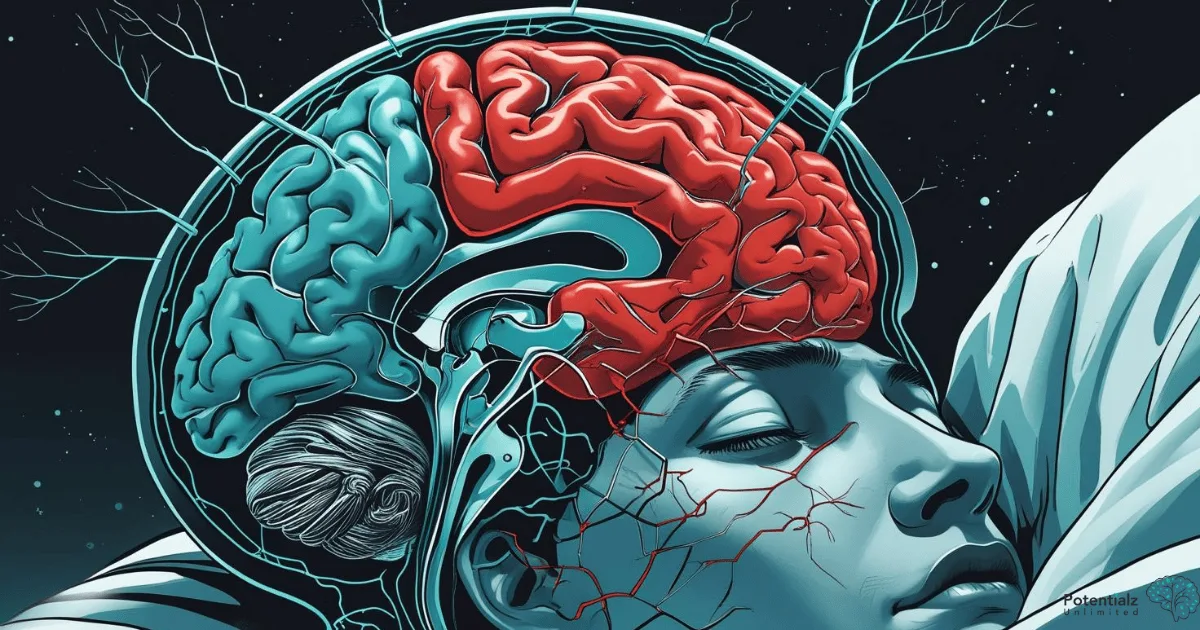 An AI generated illustration showing a cross-section of the brain during PTSD nightmares, with the amygdala highlighted in red (hyperactivity), hippocampus in blue (disrupted processing), and neural pathways between them shown as interrupted connections.
An AI generated illustration showing a cross-section of the brain during PTSD nightmares, with the amygdala highlighted in red (hyperactivity), hippocampus in blue (disrupted processing), and neural pathways between them shown as interrupted connections.
The Cycle of PTSD Sleep Disruption
Individuals with PTSD frequently have trouble falling asleep and awaken easily, often waking up many times throughout the night. Many people with PTSD also have nightmares. These issues result in disrupted, non-refreshing sleep. This creates a vicious cycle that can perpetuate PTSD symptoms:
Phase 1: Pre-Sleep Anxiety
Fear of nightmares creates anticipatory anxiety around bedtime, making it difficult to fall asleep. The bedroom may feel unsafe rather than restful.
Phase 2: Sleep Fragmentation
When sleep does occur, it’s often light and easily disrupted. The brain remains partially alert for potential threats, preventing deep, restorative sleep.
Phase 3: Nightmare Occurrence
Vivid, traumatic dreams occur during REM sleep, often waking the person in distress and fear.
Phase 4: Post-Nightmare Distress
Upon waking from nightmares, individuals may experience panic, disorientation, and difficulty distinguishing dreams from reality.
Phase 5: Sleep Avoidance
Fear of experiencing another nightmare leads to staying awake longer, further disrupting natural sleep patterns.
Research indicates that chronic nightmares in PTSD are associated with adverse consequences and decreased psychological and physiological functioning as well as disturbed sleep. Breaking this cycle requires a comprehensive approach addressing both the symptoms and underlying trauma.
Evidence-Based Treatment Approaches
Imagery Rehearsal Therapy (IRT): The Gold Standard
Results indicate that imagery rehearsal had large effects on nightmare frequency, sleep quality, and PTSD symptoms. These effects were sustained through 6 to 12 month follow-up. IRT is currently considered the most effective psychological treatment for PTSD nightmares.
How IRT Works: IRT operates on the principle that you can “reprogram” nightmares by consciously creating new, less frightening outcomes while awake. The goal is to ‘reprogram’ your nightmares to be less terrifying if and when they occur again.
The Three-Stage IRT Process:
Stage 1: Exposure and Documentation
- Write down the nightmare in detail while awake
- Include specific elements: setting, characters, sequence of events, emotions
- Focus on accuracy without trying to change anything initially
- Practice staying calm while reviewing the content
Stage 2: Rescripting and Transformation
- Identify the most distressing elements of the nightmare
- Create alternative, more positive outcomes for these elements
- Develop a new narrative that feels realistic and empowering
- Ensure the new version addresses themes of safety, control, and resolution
Stage 3: Mental Rehearsal
- Visualize the new, improved dream narrative for 10-20 minutes daily
- Practice during relaxed, wakeful states (not immediately before sleep)
- Repeat the new storyline until it becomes familiar and automatic
- Continue practice even after nightmares begin to improve
Example IRT Application:
Original nightmare: Being chased through dark hallways with no escape
Rescripted version: Being chased but finding a door that leads to a safe room where helpers are waiting, or gaining the ability to fly above the threat
One key to remember is that you don’t need to go through every single bad dream. After revising and rehearsing a few disturbing dreams, you’ll likely notice fewer other nightmares, too.

Cognitive Behavioral Therapy for Insomnia (CBT-I)
The best treatment for insomnia is Cognitive Behavioral Therapy for Insomnia, or CBT-I. This talk therapy is recommended over medication because it is more effective—CBT-I has been shown to work in multiple research studies—and has fewer side effects than medication. CBT-I improves sleep in 7 out of 10 people who complete it.
Core CBT-I Components for PTSD:
Sleep Restriction Therapy
- Limit time in bed to actual sleep time to increase sleep efficiency
- Gradually increase sleep window as sleep improves
- Avoid lying awake in bed, which can increase anxiety
Stimulus Control
- Use the bedroom only for sleep and intimacy
- Leave the bedroom if unable to fall asleep within 20 minutes
- Return only when feeling sleepy
- Maintain consistent wake times regardless of sleep quality
Cognitive Restructuring
- Challenge catastrophic thoughts about sleep and nightmares
- Replace “I’ll never get good sleep” with “Sleep difficulties are treatable”
- Address safety concerns about sleeping and vulnerability
Sleep Hygiene Education
- Optimize the sleep environment for safety and comfort
- Establish consistent pre-sleep routines
- Manage light exposure to support natural circadian rhythms
Research shows that interventions that included both imagery rehearsal and cognitive behavioral therapy for insomnia resulted in greater treatment-related improvement in sleep quality than imagery rehearsal alone.
Professional Trauma-Focused Therapies
Eye Movement Desensitization and Reprocessing (EMDR)
EMDR helps process traumatic memories by engaging bilateral brain stimulation while recalling trauma. This can reduce the emotional intensity of traumatic memories that fuel nightmares.
Cognitive Processing Therapy (CPT)
CPT addresses trauma-related thoughts and beliefs that may contribute to sleep disturbances. By challenging negative cognitions about safety and control, sleep anxiety often decreases.
Prolonged Exposure Therapy
Gradual, controlled exposure to trauma memories can reduce overall PTSD symptoms, including nightmare frequency and intensity.

Creating Your Trauma-Informed Sleep Sanctuary
The bedroom environment plays a crucial role in trauma recovery. People with PTSD may feel the need to be on guard, to protect themselves from danger. It is difficult to have restful sleep when you feel the need to be always alert or are startled easily by noise.
Physical Safety and Security
Environmental Modifications:
- Bed positioning: Place your bed where you can see the door while lying down
- Lighting options: Install dimmer switches and keep a small night light for orientation
- Sound management: Use white noise machines to mask sudden sounds that might trigger startle responses
- Temperature control: Maintain a cool, comfortable room temperature (65-68°F)
- Clutter reduction: Keep pathways clear for easy navigation if you need to get up quickly
Security Measures:
- Door locks: Ensure bedroom door can be locked from inside if needed
- Window treatments: Use blackout curtains that can be quickly opened for escape routes
- Emergency items: Keep a flashlight, water, and phone charger within reach
- Comfort objects: Include meaningful items that promote feelings of safety and connection
Sensory Comfort and Regulation
Tactile Elements:
- Weighted blankets: The gentle pressure can reduce anxiety and promote calm
- Soft textures: Use comfortable bedding that feels soothing against the skin
- Temperature regulation: Layer blankets so you can adjust warmth as needed
Aromatherapy for Trauma Recovery:
- Lavender: Promotes relaxation and may reduce nightmare frequency
- Chamomile: Calms the nervous system and reduces anxiety
- Sandalwood: Grounds the nervous system and promotes security
- Bergamot: Uplifts mood while maintaining calming properties
Always use high-quality, pure essential oils and discontinue if any scent triggers traumatic memories
Visual Environment:
- Calming colors: Choose blues, greens, or earth tones that promote tranquility
- Meaningful artwork: Display images that evoke safety, peace, and positive memories
- Natural elements: Include plants or nature imagery to promote healing
- Avoid triggers: Remove or cover items that might remind you of trauma
 The bedroom makeover makes it more conducive to sleep.
The bedroom makeover makes it more conducive to sleep.
Daily Practices for Better Sleep with PTSD
Morning Routines for Sleep Success
Light Exposure Therapy
- Get sunlight within 1 hour of waking to regulate circadian rhythms
- Spend 10-30 minutes outside or near a bright window
- Use light therapy lamps during dark winter months
- Avoid blue light filtering in the morning to enhance alertness
Movement and Grounding
- Gentle exercise: Light stretching or walking can reduce overall anxiety
- Grounding techniques: Connect with your body and present moment
- Breathwork: Practice calming breathing to start the day centered
Afternoon and Evening Strategies
Stress Management Throughout the Day
- Regular check-ins: Monitor stress levels and use coping skills proactively
- Mindfulness breaks: Brief meditation or breathing exercises
- Physical activity: Regular exercise improves sleep quality, but avoid intense workouts within 4 hours of bedtime
- Nutrition timing: Avoid large meals, caffeine, and alcohol close to bedtime
Pre-Sleep Routine (1-2 Hours Before Bed)
Technology Boundaries:
- Digital sunset: Stop using screens 1-2 hours before sleep
- Blue light filters: Use if you must use devices in the evening
- Charging station: Keep devices out of the bedroom
- News avoidance: Limit exposure to triggering content before bed
Relaxation Sequence:
- Warm bath or shower: The temperature drop afterward promotes sleepiness
- Gentle stretching: Release physical tension from the day
- Journaling: Write down worries or gratitude to clear your mind
- Reading: Choose calming, non-stimulating content
- Breathing exercises: Practice 4-7-8 breathing or progressive muscle relaxation
Bedtime Rituals for Safety and Calm
The 5-4-3-2-1 Grounding Technique
Before lying down, identify:
- 5 things you can see (comfort items, safe objects)
- 4 things you can touch (soft blanket, smooth sheets)
- 3 things you can hear (white noise, distant sounds)
- 2 things you can smell (lavender, clean air)
- 1 thing you can taste (mint tea, toothpaste)
Safety Affirmations
Develop personal statements that reinforce current safety:
- “I am safe in my home right now”
- “My trauma is in the past; I am in the present”
- “I have survived difficult things and I am strong”
- “I deserve peaceful, restorative sleep”
Managing PTSD Nightmares When They Occur
Immediate Response Strategies
Upon Waking from a Nightmare:
- Orient to reality: Look around and identify familiar objects
- Ground yourself: Feel the bed beneath you, notice your breathing
- Use self-soothing: Speak calmly to yourself about your current safety
- Avoid analyzing: Don’t try to interpret the nightmare immediately
- Stay in bed if possible: Avoid reinforcing the connection between nightmares and getting up
Progressive Muscle Relaxation for Post-Nightmare Anxiety:
- Start with toes: Tense for 5 seconds, then release
- Move upward: Calves, thighs, abdomen, chest, arms, shoulders, face
- Focus on the contrast between tension and relaxation
- End with deep breathing: 4 counts in, 6 counts out
Breathing Techniques for Trauma Recovery
4-7-8 Breathing for Immediate Calm:
- Inhale through nose for 4 counts
- Hold breath for 7 counts
- Exhale through mouth for 8 counts
- Repeat 3-4 cycles maximum to avoid hyperventilation
Box Breathing for Sustained Calm:
- Inhale for 4 counts
- Hold for 4 counts
- Exhale for 4 counts
- Hold empty for 4 counts
- Continue for 5-10 cycles
Physiological Sigh for Rapid Nervous System Reset:
- Take a normal breath through your nose
- Add a second, smaller inhale on top (double inhale)
- Long, slow exhale through your mouth
- Repeat 1-3 times for immediate calm
Advanced Nightmare Management
Lucid Dreaming Training
Some trauma survivors benefit from learning to recognize when they’re dreaming and take control of the dream narrative. This requires practice and may not be suitable for everyone.
Dream Journaling with IRT Integration
- Record nightmares immediately upon waking
- Note emotional themes and trigger elements
- Practice rescripting during the day
- Track improvements over time
When to Wake Your Partner
If you share a bed, discuss with your partner:
- Signs that you’re having a nightmare (movements, sounds)
- How they should wake you (gentle voice, light touch)
- What helps you feel safe after nightmares
- How they can support without taking on caregiver burden
 Different Nightmare Management Techniques
Different Nightmare Management Techniques
Lifestyle Factors Supporting Trauma Recovery and Sleep
Exercise and Physical Activity
Trauma-Informed Exercise Approaches:
- Start slowly: Begin with gentle activities to avoid overwhelming your system
- Choose activities you enjoy: Walking, swimming, yoga, tai chi
- Morning or afternoon timing: Avoid vigorous exercise within 4 hours of bedtime
- Listen to your body: Some days require rest, and that’s healing too
Research shows that regular physical activity:
- Reduces overall PTSD symptom severity
- Improves sleep quality and duration
- Decreases inflammation associated with trauma
- Builds confidence and body awareness
Yoga and Trauma Recovery:
Trauma-informed yoga can be particularly beneficial for PTSD survivors:
- Gentle, restorative poses promote nervous system regulation
- Breathwork integration teaches self-regulation skills
- Body awareness helps reconnect with physical sensations safely
- Community classes can provide social support (when ready)
Nutrition for Sleep and Trauma Recovery
Foods That Support Sleep:
- Tryptophan-rich foods: Turkey, milk, bananas, eggs
- Magnesium sources: Dark leafy greens, nuts, seeds, whole grains
- Complex carbohydrates: Oatmeal, sweet potatoes, quinoa
- Herbal teas: Chamomile, passionflower, lemon balm, valerian root
Foods and Substances to Limit:
- Caffeine: Avoid after 2 PM, or earlier if sensitive
- Alcohol: While it may help you fall asleep, it disrupts sleep quality and can worsen nightmares
- Heavy meals: Finish eating 3 hours before bedtime
- Sugar and processed foods: Can cause energy spikes and crashes
Timing Strategies:
- Consistent meal times: Help regulate circadian rhythms
- Light evening snack: Small protein + carbohydrate combination if hungry before bed
- Hydration balance: Stay hydrated during the day but reduce fluids 2 hours before sleep
Social Support and Connection
Building Your Support Network:
- Trauma-informed friends and family: People who understand PTSD challenges
- Support groups: Connect with others who share similar experiences
- Professional team: Therapist, physician, case manager as needed
- Peer support specialists: Individuals with lived trauma experience who are trained to help
Communication Strategies:
- Educate loved ones about PTSD and sleep challenges
- Set boundaries around sleep time and space
- Ask for specific support rather than general help
- Practice saying no to activities that interfere with sleep routines
When to Seek Professional Help
Red Flag Symptoms Requiring Immediate Attention
Seek immediate professional help if you experience:
- Suicidal thoughts or plans: PTSD nightmares are associated with increased suicide risk
- Substance abuse: Using alcohol, drugs, or medications to sleep
- Severe sleep deprivation: Less than 4 hours of sleep per night for extended periods
- Psychotic symptoms: Difficulty distinguishing dreams from reality when awake
- Self-harm behaviors: Injuring yourself during or after nightmares
When Standard Self-Help Isn’t Enough
Consider professional support when:
- Nightmares persist despite consistent self-help efforts for 6-8 weeks
- Sleep problems significantly impact daily functioning (work, relationships, health)
- Trauma symptoms worsen or new symptoms emerge
- Multiple sleep disorders are present (sleep apnea, restless leg syndrome)
- Medical complications arise from chronic sleep deprivation
Types of Professional Support
Mental Health Professionals:
- Trauma specialists: Psychologists or counselors trained in PTSD treatment
- Sleep psychologists: Specialists in behavioral sleep medicine
- Psychiatrists: For medication evaluation and management
- EMDR practitioners: Certified in Eye Movement Desensitization and Reprocessing
Medical Professionals:
- Sleep medicine physicians: For comprehensive sleep disorder evaluation
- Primary care providers: For overall health monitoring and referrals
- Neurologists: If neurological factors may be contributing to sleep issues
Specialized Programs:
- Intensive outpatient programs for severe PTSD
- Sleep disorder clinics for comprehensive evaluation
- Veteran-specific programs for military trauma
- Women’s trauma programs for gender-specific approaches
Research also shows that CBT-I reduces how many nightmares people have and the distress related to upsetting dreams, emphasizing the importance of professional treatment when needed.
Medication Considerations
Medications for PTSD Nightmares:
While behavioral interventions are preferred, medications may be helpful in some cases:
- Prazosin: Most studied medication for PTSD nightmares, though recent research shows mixed results
- Antidepressants: May reduce overall PTSD symptoms and improve sleep
- Sleep medications: Generally used short-term due to dependency risks
The failure of prazosin in the CSP trial makes behavioral therapy the treatment of choice for this disorder, highlighting the importance of psychological interventions over medication-only approaches.
Building Long-Term Recovery and Resilience
The Recovery Timeline: What to Expect
Weeks 1-4: Foundation Building
- Establishing sleep hygiene and environmental safety
- Beginning basic relaxation techniques
- Possible initial increase in sleep awareness and some continued difficulty
Weeks 4-12: Skill Development
- Implementing IRT or other specific nightmare interventions
- Developing consistent routines and coping strategies
- Gradual improvement in sleep quality and nightmare frequency
Months 3-6: Integration and Refinement
- Fine-tuning strategies that work best for your unique situation
- Building confidence in your ability to manage sleep challenges
- Addressing any remaining sleep difficulties or trauma symptoms
Months 6+: Maintenance and Growth
- Developing relapse prevention strategies
- Expanding your toolkit for life’s ongoing challenges
- Possibly helping others who are earlier in their recovery journey
Measuring Progress and Success
Quantitative Measures:
- Sleep diary tracking: Hours slept, nightmare frequency, sleep quality ratings
- Standardized questionnaires: PTSD symptom scales, sleep quality indices
- Physical health indicators: Energy levels, immune function, concentration
Qualitative Improvements:
- Increased sense of safety in the bedroom and during sleep
- Greater confidence in your ability to manage difficult symptoms
- Improved relationships due to better sleep and reduced trauma symptoms
- Enhanced daily functioning in work, social, and personal activities
Preventing Relapse and Managing Setbacks
Common Triggers for Sleep Disruption:
- Anniversary dates of traumatic events
- High stress periods (job changes, relationship issues, health problems)
- Changes in routine (travel, schedule shifts, living situations)
- Exposure to trauma reminders (news events, movies, conversations)
Relapse Prevention Strategies:
- Maintain consistent routines even during stressful periods
- Have a crisis plan with specific steps to take when nightmares return
- Keep your support network informed about your ongoing needs
- Practice self-compassion - setbacks are normal parts of recovery
Early Warning Signs:
- Increased anxiety about bedtime or sleep
- Return of avoidance behaviors around sleep
- Changes in nightmare content or frequency
- Deterioration in daily functioning due to sleep problems
 A Journey of Recovery from PTSD Nightmares
A Journey of Recovery from PTSD Nightmares
Self-Help Strategies You Can Implement Tonight
Immediate Actions for Better Sleep
Tonight’s Sleep Preparation:
- Create a “worry time” 2 hours before bed - write down concerns and set them aside
- Prepare your environment using the safety strategies outlined above
- Practice one new breathing technique from this guide
- Set realistic expectations - improvement takes time, and every small step counts
This Week’s Goals:
- Establish one consistent bedtime routine element
- Try journaling about sleep experiences without judgment
- Implement basic sleep hygiene improvements
- Practice grounding techniques during the day to build familiarity
This Month’s Objectives:
- Begin IRT with one recurring nightmare
- Optimize your sleep environment for safety and comfort
- Develop your support network by talking to trusted friends or family
- Consider professional consultation if self-help strategies aren’t sufficient
Emergency Coping Kit for Difficult Nights
Create a bedside “toolkit” containing:
- Written grounding instructions and safety affirmations
- Essential oils or other calming scents
- Comforting objects that promote feelings of safety
- Emergency contact information for crisis support
- Breathing exercise cards with simple instructions
- A gratitude journal to shift focus when needed
Test Your Knowledge: PTSD Sleep Management Quiz
Question 1: Multiple Choice
According to current research, what is considered the most effective psychological treatment for PTSD nightmares?
a) Medication therapy with prazosin
b) Imagery Rehearsal Therapy (IRT)
c) Sleep restriction therapy
d) Exposure therapy
Question 2: True or False
Sleep problems in PTSD are considered a secondary symptom that will resolve once other PTSD symptoms improve.
Question 3: Fill in the Blank
The three main stages of Imagery Rehearsal Therapy are: _______, _______, and _______.
Question 4: Short Answer
Explain why creating a sense of safety in the bedroom environment is particularly important for trauma survivors, and name two specific modifications that can help.
Question 5: Application
Your friend with PTSD tells you they’ve been avoiding sleep for several nights because they’re afraid of having nightmares. Using information from this guide, suggest three specific strategies they could try tonight to feel safer about sleep.
Answer Key:
- b) Imagery Rehearsal Therapy (IRT) - Research shows IRT has large, sustained effects on nightmare frequency, sleep quality, and PTSD symptoms.
- False - Sleep problems in PTSD are actually considered part of the disorder itself, not secondary symptoms, and often require direct treatment.
- Exposure, Rescripting, Rehearsal - These three stages help individuals rewrite nightmare content and practice new, less distressing dream narratives.
- Sample answer: Trauma survivors may feel vulnerable during sleep and need environmental safety to allow their nervous system to relax. Modifications could include: positioning the bed to see the door, using layered lighting options, installing locks, keeping comfort objects nearby, or using white noise to mask startling sounds.
- Sample response: Tonight, your friend could: (1) Create a simple safety check routine - looking around the room and identifying 5 safe objects before lying down, (2) Practice 4-7-8 breathing while lying in bed to calm their nervous system, (3) Write a brief note to themselves affirming their current safety and place it where they can see it. Tomorrow, they should consider reaching out to a trauma-informed therapist for additional support.
Key Takeaways: Reclaiming Peaceful Sleep After Trauma
Bottom Line Up Front: PTSD nightmares are treatable symptoms with evidence-based interventions that can significantly improve sleep quality and overall recovery. While the journey requires patience and often professional support, peaceful sleep is achievable for trauma survivors.
Essential Principles for Success:
- Sleep problems in PTSD require direct treatment - they don’t automatically resolve when other symptoms improve
- Environmental safety is foundational - creating a trauma-informed sleep space supports nervous system regulation
- Imagery Rehearsal Therapy is the gold standard for nightmare treatment with strong research support
- Professional help is often necessary - trauma-informed sleep treatment can accelerate recovery
- Recovery is possible - with appropriate intervention, most people experience significant improvement
Your Next Steps:
- Tonight: Implement one environmental safety modification and practice a breathing technique
- This week: Begin tracking your sleep patterns and nightmare frequency without judgment
- This month: Consider consulting with a trauma-informed sleep specialist or therapist
- Ongoing: Remember that healing takes time, and every step toward better sleep is progress worth celebrating
Remember: You survived your trauma, and you can reclaim peaceful sleep. Nightmares are symptoms, not life sentences. With the right tools, support, and patience with yourself, restful nights and renewed days are within reach. Your courage in seeking help and implementing these strategies is part of your healing journey.
The path from trauma to peaceful sleep isn’t always linear, but it leads to a place where rest comes naturally and dreams can return to their healing purpose. You deserve restorative sleep, and with evidence-based strategies and appropriate support, it’s absolutely achievable.
References
- Augedal, A. W., Hansen, K. S., Kronhaug, C. R., Harvey, A. G., & Pallesen, S. (2013). Randomized controlled trials of psychological and pharmacological treatments for nightmares: A meta-analysis. Sleep Medicine Reviews, 17(2), 143-152.
- Casement, M. D., & Swanson, L. M. (2012). A meta-analysis of imagery rehearsal for post-trauma nightmares: Effects on nightmare frequency, sleep quality, and posttraumatic stress. Clinical Psychology Review, 32(6), 566-574.
- El-Solh, A. A. (2018). Management of nightmares in patients with posttraumatic stress disorder: Current perspectives. Nature and Science of Sleep, 10, 409-420.
- Germain, A. (2013). Sleep disturbances as the hallmark of PTSD: Where are we now? American Journal of Psychiatry, 170(4), 372-382.
- Haeyen, S., van Hooren, S., van der Veld, W. M., & Hutschemaekers, G. (2018). Imagery rehearsal based art therapy: Treatment of post-traumatic nightmares in art therapy. Frontiers in Psychology, 9, 628717.
- Krakow, B., & Zadra, A. (2006). Clinical management of chronic nightmares: Imagery rehearsal therapy. Behavioral Sleep Medicine, 4(1), 45-70.
- Perogamvros, L., Castelnovo, A., Samson, D. R., Baril, A. A., Bargiotas, P., Nieminen, J. O., … & Schwartz, S. (2022). Enhancing imagery rehearsal therapy for nightmares with targeted memory reactivation. Current Biology, 32(22), 4808-4816.
- Raskind, M. A., Peskind, E. R., Chow, B., Harris, C., Davis-Karim, A., Holmes, H. A., … & McFall, M. E. (2018). Trial of prazosin for post-traumatic stress disorder in military veterans. New England Journal of Medicine, 378(6), 507-517.
- Sleep Foundation. (2024). PTSD and sleep. Retrieved from https://www.sleepfoundation.org/mental-health/ptsd-and-sleep
- U.S. Department of Veterans Affairs. (2023). Sleep problems and PTSD. PTSD: National Center for PTSD. Retrieved from https://www.ptsd.va.gov/understand/related/sleep_problems.asp
- Yücel, D. E., van Emmerik, A. A., Souama, C., & Lancee, J. (2020). Comparative efficacy of imagery rehearsal therapy and prazosin in the treatment of trauma-related nightmares in adults: A meta-analysis of randomized controlled trials. Sleep Medicine Reviews, 50, 101248.
Need Professional Support?
If you're experiencing mental health concerns, our team is here to help.